A Blood Test to Predict Alzheimer’s Disease – Too good to be true?

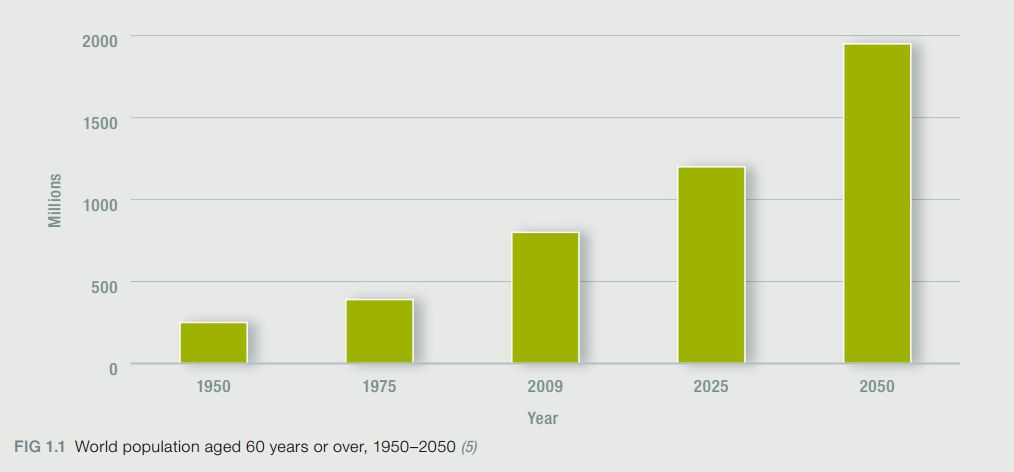
The World Health Organisation (WHO) has estimated that Alzheimer’s disease currently affects 35.6 million people worldwide. This number is expected to double by 2030 and by 2050 the number affected by Alzheimer’s is expected to reach 115.4 million. The number of new cases of dementia is over 7 million per year worldwide, which is approximately one new case every 4 seconds. Unfortunately, at the moment of writing, there is no cure for Alzheimer’s. We are not close to fully understanding how this disease begins and progresses in the brain but we are advancing our knowledge every single day through fundamental research in the lab.
Not all studies investigating Alzheimer’s disease are based in fundamental biology labs, there are many public health studies which investigate large populations of people with different stages of dementia in order to try and find correlations in their lifestyles which could suggest a greater chance of developing dementia in old age. These studies have gone a long way to develop our knowledge of some risk factors associated with Alzheimer’s disease. The first risk factor seems quite obvious, it’s Age; the older you are the higher your risk of Alzheimer’s disease. From these public health studies we also know that smoking, hypertension and type 2 diabetes all increase the risk of developing Alzheimer’s disease.
What’s also frustrating is that we also lack definite diagnostic tests which can tell us if somebody is at risk of developing dementia. There exist some genetic tests which are not widely used, one of these tests for the APOE-e4 gene, if you are a carrier of this gene this means that you are at risk of developing Alzheimer’s but it’s not definitive, you can carry the gene and never develop the disease. The other test is for autosomal dominant Alzheimer’s disease (ADAD), this involves mutations in one or several genes and is responsible for the ‘familial Alzheimer’s’ therefore if you have one of these mutations you are certain to get Alzheimer’s disease. This familial Alzheimer’s is quite rare and accounts for less than 5% of all cases.
Alzheimer’s is a growing burden on society and there is a lot of effort behind funding research into this disease. So it’s understandable that there was a lot of excitement when a recent paper was published in Nature Medicine showing a potential blood test which can predict Alzheimer’s disease. This study enrolled people aged 70 and over who were followed over 5 years in total. Before I go any further it’s important to mention that this paper is more like a proof of principle and has yet to be developed and tested on a wider population, which means this test is not going to appear on your shelves in the coming months. A lot more work is necessary before we can even think of bringing this test to clinical trials which are extremely expensive and have a very high rate of failure.
In this study, participants were divided into healthy or mild-cognitive impairment (Alzheimer’s group). During the study, it was found that some of the participants who began in the healthy group developed Alzheimer’s disease, while others remained healthy throughout. The researchers screened their blood samples for some biomarkers which would allow them to diagnose Alzheimer’s before the actual onset of the disease. This arduous task, beginning with many thousands of possible targets, revealed that only a handful of possible biomarkers that seemed to be correlated with those who developed Alzheimer’s, some of these biomarkers were increased and others decreased compared to people who never developed Alzheimer’s. In the end, the researchers were able to identify a small group of 10 biomarkers (some of which were phospholipids – which among other roles are important for maintaining normal cell membranes) whose levels were changed in the group of people who had developed Alzheimer’s compared to the healthy control group of participants.
The authors suggest that these biomarkers have the potential to determine who will develop Alzheimer’s disease before they actually show any clinical symptoms, such as memory trouble. They hypothesise that changes in the levels of these phospholipids detected in the blood may have a direct impact on the structural integrity of neurons in the brain.
However, there are two major drawbacks; first this test can only tell us if a person will develop Alzheimer’s 2-3 years before the disease takes hold; and second this test is only accurate 90% of the time.
Before I discuss these drawbacks I would first like to point out something else which surprised me. Even today it is difficult to distinguish between different forms of dementia – Alzheimer’s disease is only one form, there are many others. Normally, to say with a relatively high certainty that a person has Alzheimer’s disease it is necessary to carry out cognitive tests, then different brain scans are required to see if there is atrophy of certain brain areas and also to see if there are plaques in the brain, and finally it is necessary to take a sample of cerebrospinal fluid to measure the levels of Amyloid-b and Tau proteins (these two proteins which have normal physiological functions in the healthy brain, dysfunction in Alzheimer’s disease and are believed to be responsible for many of the effects of the disease, such as cell death and inflammation). Even with all of these tests, the one sure-fire way of knowing if somebody had Alzheimer’s disease is taking a look at their brain post-mortem. Researchers in this study imply that those patients with mild-cognitive impairment have Alzheimer’s disease, but I don’t believe they have done the necessary testing to rule out the possibility that these people had another form of dementia. They only carried out the cognitive testing.
Why didn’t they do these other tests, you might ask? Well it’s likely due to the cost of these procedures. Brain scans and taking cerebrospinal fluid samples are expensive, time-consuming and are quite invasive. It can be difficult to recruit patients if you plan on carrying out procedures like these. All the more reason for interest in a potential blood test for Alzheimer’s, its quick inexpensive and should be relatively easy to carry out.
The fact that this test is can only predict if a person will develop Alzheimer’s 2-3 years in advance has been criticised for many reasons including ethical reasons. There is no cure for Alzheimer’s disease, so is it ethical to tell these people when there is absolutely nothing they can do about it? This question is very difficult to answer. Personally, if this test was available, I think people should have the choice. This will give them 2-3 years to make necessary arrangements and make the most of the time they have before the disease progresses. A couple of years is not much but imagine where this may lead… This is a great start and from here it’s not impossible to imagine that future studies will find more robust biomarkers which will give us enough time to make lifestyle changes needed to avoid developing Alzheimer’s disease. I would like to remind you now that we already know a few risk factors associated with this disease, as I mentioned at the beginning of this piece.
The fact that this test, at its current state, is accurate 90% of the time is already quite good for a test at this level, its nowhere near what is needed for a marketable product but it’s a good indication of the strength of this test and we should be hopeful that this will be developed further and maybe lead to an even better diagnostic for those likely to develop Alzheimer’s disease.
The media has jumped on this story and why not? I think it’s really great that science is becoming increasingly mainstream. However, we need to be cautious when interpreting these results and this time I have to say that most of the media reports I read online have indeed been cautious whether that be due to the low number of people tested or the efficacy of this test.
So overall, I wouldn’t get overexcited about this new discovery but it’s a welcome step forward in the development of a non-invasive, inexpensive test to predict Alzheimer’s disease and this in itself should be praised.
